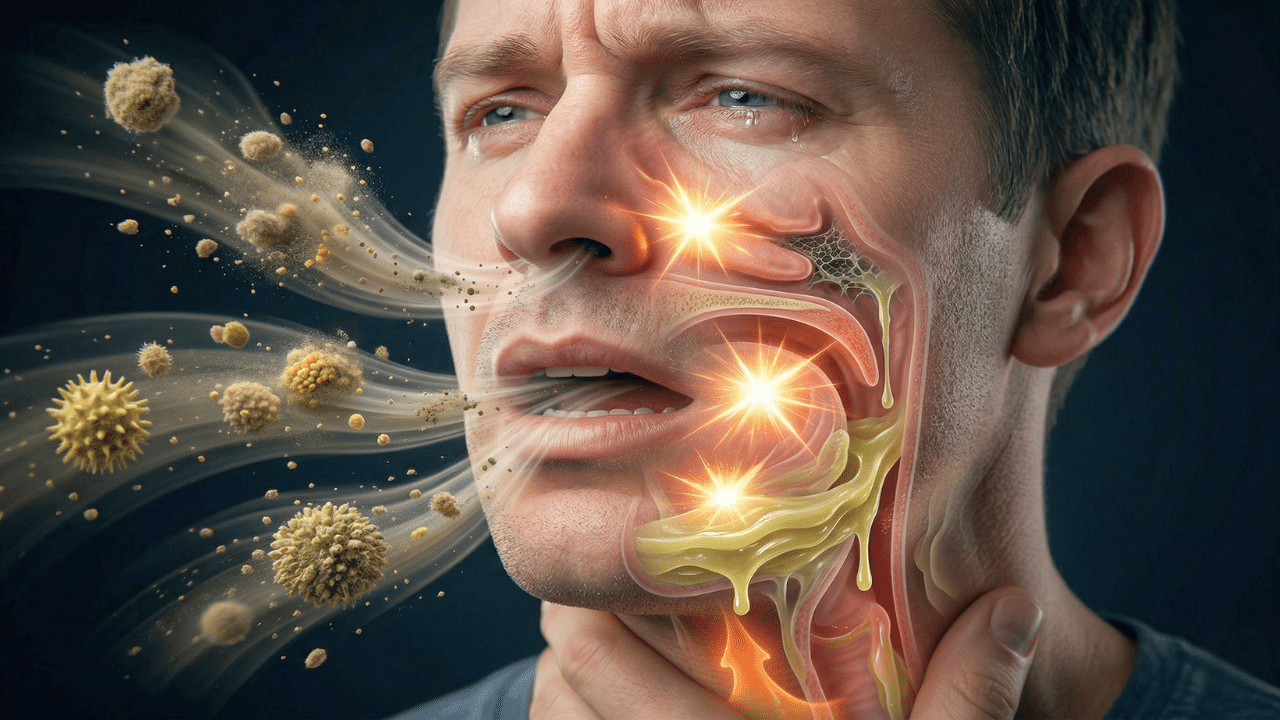
Do you feel a firm lump in the back of your throat? That annoying, and sometimes painful, feeling of needing to clear your voice all the time? If so, you are not alone. Chronic mucus, also known as postnasal drip, affects millions of people and can seriously disrupt your quality of life. Let’s be honest, the first thing we usually do is reach for medication to stop the symptoms. But here’s the problem: Conventional treatments, such as antibiotics, are often only a temporary fix. Worse still, they can cause side effects, weaken your immune system, or encourage the growth of antibiotic-resistant fungi and bacteria.
Today, we break that cycle. We’ll get to the root of the problem. Stay with me, because we’ll break down why your body is producing this excess mucus and how you can treat it effectively, naturally, and for good. Before we get started, an important reminder: This content is intended for informational and educational purposes only. It does not replace the advice of a physician and cannot provide you with personalized medical advice. Always consult your doctor before making any changes to your treatment plan. (Based on Sento Farmacéutico insights)
Key takeaways
- Overcome symptoms: Chronic mucus is often a sign of a deeper problem. Simply suppressing it with medications may not solve the underlying problem and can lead to other complications.
- Four common culprits: The most common and often overlooked causes of persistent mucus are gastroesophageal reflux (even the silent type), chronic sinus infections (biofilms), hypothyroidism, and hidden allergies or allergies.
- Low stomach acid may be the problem: Contrary to popular belief, reflux is not always caused by too much stomach acid. For many, the cause is an insufficient number of the esophagus, which prevents the esophageal valve from closing properly.
- Powerful natural solutions: Strategies such as nasal irrigation, dietary changes (such as experimental elimination of dairy products), targeted supplements, and intermittent fasting can address the root causes and provide lasting relief.
1. Sudden cause: gastroesophageal reflux
The first and perhaps most surprising reason is… Gastroesophageal refluxor esophageal reflux. Reflux occurs when stomach acid moves up the esophagus and into the throat. This leads to irritation and inflammation of sensitive tissues, and your body produces mucus as a defense mechanism. The result? Sore throat, chronic cough, and constant feeling of a lump. The standard treatment for this condition is a class of medications called proton pump inhibitors (PPIs), known as omeprazole, esomeprazole, and pantoprazole. Millions of people take it long term.
However, recent studies show that taking these medications for months or years can have serious consequences, including vitamin deficiencies, bone problems, changes in the gut microbiome, and even a rebound increase in reflux when you stop taking them. But here’s a twist: Sometimes reflux isn’t caused by too much acid; It happens because you have too little. This concept, known as hypochlorhydria, is not formally recognized in conventional medicine and human clinical evidence remains limited, but it is a physiologically sound hypothesis widely used in functional and integrative medicine. The lower esophageal sphincter, the valve that separates the esophagus from the stomach, needs a highly acidic environment to close tightly. If your stomach is not acidic enough, the valve can remain partially open, allowing the contents to back out.
How do you know if this is your situation? You can try a simple, indicative (not diagnostic) test. Try taking a tablespoon of apple cider vinegar diluted in a glass of water before a meal. If you notice an improvement in your symptoms, it may be a sign that you have low stomach acid. Remember, this is a sign, not a diagnosis. Another option used in functional medicine is betaine hydrochloride (HCl), a supplement that provides hydrochloric acid. It is taken with meals to help acidify the stomach. But be careful, this is powerful stuff. If you have an ulcer or active gastritis or are taking anti-inflammatory medications, do not attempt this without medical supervision.
2. Hidden invaders: chronic sinus infections and biofilms
The second main cause can be chronic sinus infections. I’m not talking about severe infections that resolve after a week of antibiotics; I’m talking about the ones that last for months or even years. This is where biofilms come into play. Imagine a fortified city of bacteria, fungi, and other microorganisms clinging to the walls of your sinuses. They build a kind of protective mucus shield around themselves. Inside this shield, they are safe. Antibiotics can’t penetrate it well, and your immune system can’t reach it. Therefore, they continue to generate inflammation and mucus that constantly drips into the back of the throat.
These biofilms explain why some sinus infections do not heal completely. You may feel better after a course of antibiotics, but after weeks, you’re back to where you started. If you continue this cycle, you may end up developing resistant bacterial strains. To solve this problem, we resort to nasal irrigation with saline solution, popularly known as a neti pot. A Neti pot is a small teapot-shaped bowl used to pour salt water through one nostril until it flows out the other nostril. It sounds strange until you try it, and it works through two mechanisms. First, it’s mechanical: the flow of water removes mucus, allergens and parts of those biofilms. Second, it’s biological: salt stimulates cilia, the tiny hairs that line the respiratory system and whose job it is to expel mucus. When there is inflammation or infection, the cilia become paralyzed or move very slowly. Salt reactivates them.
It is necessary to use seawater or isotonic saline solution. Never use tap water without boiling and cooling it first, as it may contain harmful microorganisms. If you have an active infection, you can use solutions with a higher salt concentration, known as hypertonic solutions. If you have had unexplained mucus for several months, try using a Neti pot for two weeks. Many people notice a huge difference within days.
3. Neglected relationship: hypothyroidism
The third reason is one that often flies under the radar: HypothyroidismOr hypothyroidism. This is especially important because it can affect many people who have suffered from chronic mucus for years without knowing the cause. The thyroid gland produces hormones that regulate the metabolism of the entire body. When it works too slowly, everything slows down, including the system that drains mucus from your sinuses and throat. The cilia we just talked about are also affected. With hypothyroidism, their movements become slow, and mucus accumulates.
What are the warning signs? Constant fatigue, unexplained weight gain, dry skin, cold intolerance, and yes, thick mucus that won’t go away, especially in the morning. If you have these symptoms along with chronic mucus, ask your doctor to give you a complete thyroid panel to get a clear picture of your thyroid function.
4. Exaggerated immune reaction: allergy
Finally, we have sensitivity. Allergies are an uncontrolled response of your immune system to harmless substances such as pollen, dust mites, or certain foods. This response generates inflammation, histamine, and mucus. First, there is environmental allergy to pollen, dust, and mites. These are evident in the spring but can be a problem year-round if you live with allergens in your home. If you suspect this is your condition, an allergist can confirm this with skin tests or specific blood work.
But there’s a type of allergy we often underestimate: food allergies. The most discussed in this context is dairy products. Here I want to be honest with you because we are entering the area with controversial evidence. More rigorous studies have not found that dairy increases objective mucus production in the general population. However, in functional medicine, it is clinically observed that there are sensitive individuals whose symptoms improve clearly after removing dairy. The hypothesis points to beta-casomorphin 7, a peptide that may be released from some milk proteins and can increase the density of secretions in susceptible people. Although the human evidence is still weak and it’s not a universal problem, if you have this problem and can’t find the cause, a one-month dairy-free trial is a completely harmless test that can give you valuable information about your body.
Other foods that can contribute to sensitive people include refined sugar, which can increase Candida and cause dysbacteriosis; Gluten in people with allergies. Alcohol irritates and dries the mucous membranes.
Beyond the Big Four: Other Powerful Strategies
In addition to what you remove, what you add is also important. Intermittent fasting can be very beneficial, as giving your digestive and immune systems a rest allows the body to focus on cleaning house. You do not need to fast for a long time. Starting with 12-14 hours without eating and then gradually increasing to 16 hours is sufficient for most people. To strengthen your immune system, vitamin D, vitamin C and zinc are essential. Garlic, with its antiviral, antimicrobial, and biofilm-destroying properties, is also an excellent addition. And don’t forget ginger, a natural first-line anti-inflammatory.
Listen to your body
Don’t live for years with a problem that has a solution. Don’t just cover up symptoms with temporary treatments. Your body is sending you signals, and it’s time to listen. By investigating these potential root causes, you can take control of your health and finally find lasting relief from that persistent lump in your throat.
source: Cento Pharmaceutical